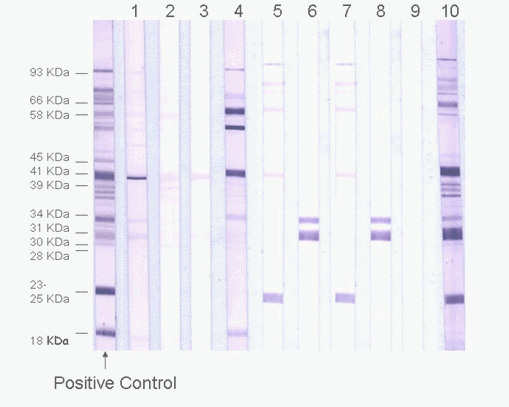
But in Lyme disease, this does not necessarily hold true. By that logic then, someone who has an IgM positive test would suggest his or her exposure to the Lyme organism was recent and someone with an IgG positive test would indicate a past infection. The CDC does not recommend doing a Lyme Western Blot IgM test on anyone whose illness occurred within the past month.Ĭonventional immunology teaches that the immune system will undergo a predictable immune response after exposure to a microbe, with IgM being the first antibody to respond to an infection, followed by the production of IgG in later stages of the illness. If someone has at least 5 out of 10 antibodies for IgG or 2 out of 3 antibodies for IgM, then the Lyme Western Blot is considered positive. The Lyme Western Blot looks at a series of specific antibodies against the Lyme organism for both IgG and IgM. If this test is positive, then a second test called a Lyme Western Blot should be run to confirm the results of the first test. The first step is to run a Lyme antibody blood test, which measure two types of antibodies against Lyme disease (immunoglobulin G or IgG and immunoglobulin M or IgM). The current recommendation by the CDC for someone who is suspicious of having Lyme disease is to run a two-step process. Here is a brief excerpt from my upcoming book on Lyme disease, “ The Lyme Solution: A 5-part Plan to Fight the Inflammatory Auto-Immune Response and Beat Lyme Disease”. Now that it is 25 years later, we have learned a great deal about Lyme disease and the pitfalls of Lyme testing have been revealed. When I was working as a microbiologist in the early 1990’s, Lyme testing was still pretty new and we didn’t know much about Lyme disease and all of the nuances of testing that would soon follow. Ingels spoke at a past Restorative Medicine Conference and is on the Scientific Advisory Board of the Restorative Medicine Herbal Certification program. The test is the same regardless of the stage of Lyme disease. If you suspect you are experiencing symptoms of late-stage Lyme disease, it makes sense to talk to your doctor about getting tested. It is much less commonly used as the bacteria are most likely to bind to joint and nerve tissues and more difficult to detect.įor more on the Lyme testing process as defined by the CDC, check out this flow chart. Alternatively, the polymerase chain reaction (PCR) is a highly sensitive test that detects DNA from the Borrelia bacteria in fluid drawn from an infected joint (typically synovial or cerebrospinal fluid).Together these tests are known as the ELISA/Western Blot. The Western blot detects antibodies to several proteins of B. The western blot is usually run as a second-stage to confirm the diagnosis following a positive ELISA result.burgdorferi and, if positive, is followed up by the Western Blot test. The Enzyme-linked immunosorbent assay or ELISA is the first step.The following tests are FDA-approved for diagnosis: There is much debate over the accuracy and reliability of the laboratory tests and the likelihood of false positives and false negatives. Lyme disease is typically assessed based on clinical diagnosis, in combination with laboratory tests. What does this mean for you? By all means, if your doctor recommends a test, get the test. In other words you could have Lyme but the test results will still come up negative. It can take your body up to two months to develop enough antibodies to be detected by these tests. Therefore a blood test at this time will often appear negative. However, with early-stage Lyme your antibodies may not have had time to develop in your body. This bacteria is called Borrelia burgdorferi, or Bb. The current laboratory diagnostic tests for Lyme disease are blood tests to detect the antibodies created by your body to fight and kill the bacteria that causes Lyme.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
